Sopris Health, an intelligent clinical operations platform that enables providers to focus on human conversations while benefiting from the support of intelligent systems, today launched a new chat-interface documentation solution that delivers a clinic note in 45 seconds or less.
“After a year in clinics across the country, tens of thousands of clinic notes and working alongside some of the most reputable medical institutions in the country, Sopris Assistant has demonstrated we’re able to complete documentation in between visits, allowing clinicians to finalize a clinic note before walking into the next exam room,” said Patrick Leonard, CEO and co-founder, Sopris Health. “Delivering real value to our customers means delivering a clinic note in the time it takes to move onto their next patient – 45 seconds or less – without the cognitive load.”
Now available on iOS to U.S. physicians and healthcare providers, “Sopris Assistant” proved in clinics to create a time reduction and ease of use unparalleled by other documentation solutions. It also drove workflow efficiencies and significantly lessened the feeling of burnout.
Brian Bristol, NP-C, and owner/operator of two Van Nuys Urgent Care facilities, said: “My interest in the Sopris Assistant was really born out of necessity, as I needed a complete documentation solution natural to my workflow, but also aware of the patient experience. I see the Sopris Assistant delivering time savings, making it possible for me to stay on top of documentation during the day without sacrificing time with patients, staff or my family. I’m able to reinvest that time into patient education, operational needs and even personal interests.”
Sopris Health is co-founded by Dr. John Froelich, a practicing orthopedic surgeon who also serves as chief medical officer: “Sopris Assistant is a response to the reality that many physicians don’t want documentation to be a part of their exam room encounter, but their hands historically have been tied with outdated, cumbersome and expensive technology solutions. Sopris Health’s clinical advisory board leverages the medical expertise of specialty clinicians with deep knowledge, which in turn enables Sopris Assistant to create palpable improvements for physicians, organizations, and the patients they serve.”
How “Sopris Assistant” Works
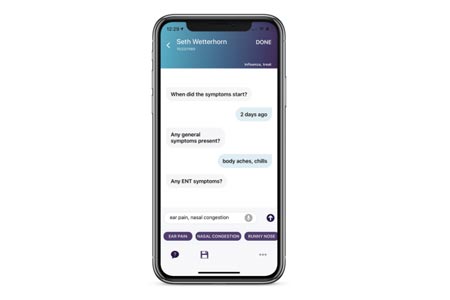
The new Sopris Assistant doubles down on a mobile experience outside the confines of an exam room, asking a few key questions in a unique chat interface.
“Throughout our onsite clinic experience with providers, we’ve observed a variety of scenarios in a variety of specialties where practitioners chose to keep technology out of the room or chose to leave part of the clinic note out of the patient conversation,” said Leonard. “If scribes need to ask a handful of questions after physicians see a patient, so will a technology. The Sopris Assistant is trained to know what questions to ask by specialty, by visit type, by note type in the simplest exchange possible.”
Providers use face or touch to securely authenticate and open the Sopris Assistant app, then tap the selected patient from a list imported via EHR integration. The Sopris Assistant walks the provider through an interactive chat interface, asking to:
- Select the type of visit – a visit model created and vetted by specialty
- Answer minimal questions via voice, text or trained “chips” that intuitively suggest appropriate, common answers – Sopris Assistant continually learns over time, making new suggestions specific to the user
- Review the clinic note automatically generated by Sopris Assistant and submit to EHR
Authoritative Interface
The Sopris Health team worked closely with its clinical advisory board to train the assistant to know the questions it needs to ask and to know how to complete the documentation.
The broad expertise helped underscore the quality of content and experience, ultimately helping to release a product that addresses these major components:
- Real-time and fully automated: Sopris Assistant is a fully automated digital assistant for medical documentation.
- Conversation data alone is insufficient: Sopris Health studied tens of thousands of notes generated by healthcare providers on its AI platform and found in 100 percent of the notes, humans were required to add content to each clinical note after the exam. The patient-provider conversations didn’t contain necessary information to generate complete clinical notes, making ambient listening a useful feature, not a complete product.
- Voice + Screen: Sopris Health spent time in clinics and specialties across the country, the experience of which demonstrated the combination of voice and select screen taps is optimal for speed and accuracy.
- Provide actual ROI: Sopris Assistant compresses 5-10 minutes of documentation per visit down to 45 seconds or less – the time it takes to walk from one exam room to the next. Instead of 2 hours of documentation after clinic or pajama time at home, a complete note is submitted by the provider to the EHR before stepping foot in the next exam room – with only a positive impact to patient experience, patient panel and workflow.
Experience with the app is only a portion of the overall relationship.
“It’s not uncommon for us to hear from a prospective customer at 10 p.m. after another evening of missed personal priorities in the name of pajama time,” said Leonard. “We know providers are desperate for a solution that mitigates today’s demands, immediately providing real value, real time savings. Their need is palpable and we push ourselves to onboard them within days.”
For more information on the new Sopris Assistant or the company overall, visit www.SoprisHealth.com.